The most common ways to improve patient safety in hospitals are following guidelines and taking precautions to avoid bacterial and viral infections. Guidelines and precautions include barriers, handwashing, and screening for resistant germs. Here are some patient safety tips mentioned for the hospitals to ensure each patient is safe in a highly susceptible environment.
Guidelines
The Guidelines for Patient Safety in Hospitals provide important information about preventing harm to patients. These guidelines are designed to help prevent problems by implementing and enforcing best practices in patient care.
While the guidelines are widely used, you should improve their rigor. The Guidelines for Patient Safety in Hospitals are not just information; they also serve as a basis for policy, planning, and evaluation. Developing quality guidelines requires a process of systematic research and development. This methodology must be divided into steps that you can summarize in a checklist. The development process should be based on evidence-based recommendations and the best available research.
The implementation process should be based on several factors such as identifying the target audience, selection of topic, such as diagnosis of chronic obstructive pulmonary disease. Moreover, the beneficiaries and other stakeholders involved should be identified. The guidelines should also be implemented in the relevant settings, with a proper process followed for implementation. This may include a clear description of the process.
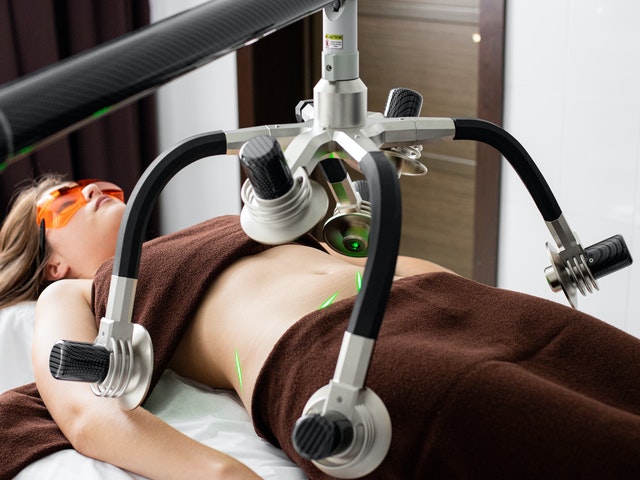
On the other hand, professional societies should be active leaders in patient safety. These societies should communicate patient safety issues to their members and integrate patient safety into their training programs. They should collaborate with physicians, pharmacists, patients, and consumers to promote safety and must work with other healthcare providers to establish appropriate responses to postmarketing surveillance.
Barrier Precautions
The Enhanced Barrier Precautions for Hospitals (EBP) are designed to help prevent the spread of medically-related infections. These guidelines recommend using PPE for all personnel who may be exposed to a particular infection, regardless of their role. These guidelines are different from Contact Precautions, which recommend using PPE based on expected exposures to blood and body fluids.
For example, Enhanced Barrier Precautions recommend using PPE in activities that involve high contact with residents. High-contact resident care activities are associated with a higher risk of MDRO transmission because the MDROs are transferred from patients’ skin to gloves and gowns.
The use of barrier protection is also necessary on non-critical surfaces. These surfaces are a source of caregiver-object-patient pathogen transmission and frequently contact hands or instruments, which may be contaminated with potentially infectious materials. In addition, these surfaces may become contaminated with potentially infectious materials during patient care.
To reduce the risk of transmission, you should use barrier protection on non-critical surfaces and change barrier protection between patients. Additionally, all medical waste should be disposed of as if it were infectious.
The Enhanced Barrier Precautions for Hospitals will replace the CDC Guideline for Isolation Precautions. It also supersedes the Guideline for the Management of Multidrug-Resistant Organisms (MDRO) in Healthcare Settings and requires healthcare personnel to undergo training in the latest guidelines on infection control. Moreover, the Enhanced Barrier Precautions for Hospitals will become mandatory in New York State in 2019.

Screening for resistant germs
One way to help prevent the spread of bacteria and germs is to know what anti-germ measures healthcare professionals are taking. The majority of bacteria that cause antibiotic-resistant infections can be found in hospitals.
Hospitals have high rates of exposure to antibiotics and frequent hand-to-hand care and close contact with patients. Because of these factors, hospitals are considered to be breeding grounds for the majority of antibiotic-resistant germs.
Antibiotic-resistant germs are a problem that has led to increased patient complaints and even deaths. To combat this problem, healthcare facilities routinely screen their patients for MRSA and other multidrug-resistant bacteria.
Screening for these germs is a good way to prevent the spread of infections, and it may help improve patient care. The Swedish government has led the way in antimicrobial resistance policies, including active “search and destroy” screening. The Swedish National Institute of Health and Welfare (NIH) has included MRSA and Vancomycin-Resistant Enterococci on their list of reportable multidrug-resistant bacteria.
Furthermore, the latest study found that about six percent of patients who did not have the presence of MDROs at the start of their hospitalization tested positive for them later. In addition, one-fifth of the objects in patient rooms had superbugs.
Although it may be tempting to think that resistant germs in a hospital indicate that the patient has already been infected, there is no certainty that they are susceptible to infection. The study also found that hand-to-hand contact with patients is the primary means of spreading these germs.
Handwashing
The Vienna General Hospital’s handwashing experiment illustrates the importance of handwashing as a patient safety tip. While handwashing practices have proven effective, many physicians and other health professionals resist the idea, citing the risk of the implication that they are to blame for causing a patient’s illness.
The role of handwashing in patient safety in hospitals is crucial. In addition to teaching patients the proper technique, nurses can also educate hospital workers. Teaching people to wash their hands frequently is essential to reducing the risk of infection.
The Centers for Disease Control (CDC) has a website that encourages proper hand washing in healthcare settings. It explains that hand washing can help stop the spread of HAI.
However, hand washing is not the only way to keep the patients safe. Besides hand washing, other patient safety tips include not touching your own nose, mouth, or eyes.
Social (physical) distancing

Implementing social (physical) distancing as a hospital patient safety tip has several advantages. The CDC has guidelines on using personal protective equipment in hospitals, and it recommends that patients wait in their cars rather than in the waiting rooms. Waiting rooms should be kept free of magazines and toys. However, if there are any, you should regularly disinfect them. Facilities should develop a cleaning schedule and checklist and document the steps taken.
Regardless of the setting, social (physical) distancing should be a hospital safety tip. Using technology to eliminate the waiting room can improve patient safety. Digital check-in can comply with the social distancing guidelines. Using software to manage patient intake forms is a good option since it enhances safety and saves office staff time.
Keeping a distance of six feet between patients is another important patient safety tip. Coughing without covering your face can transmit the infection to others. Keeping a safe distance from patients can help slow the spread of COVID-19. People need to follow these guidelines if they are in a community with a high risk of disease.
Financial incentives
A study at Duke University Hospital examined the impact of financial incentives on patient safety in hospitals. Using an incentive of $200 to report two safety events a year, more than half of eligible trainees reported two or more safety events per year. The study tracked how many safety reports were submitted during the 2014-2015 academic year. The study found that more than half of eligible trainee physicians reported a safety event. And the rate remained high in the following academic years.
A new study found that financial incentives for patient safety are not linked to a decline in healthcare-associated infections (HCAIs). While financial incentives for patient safety in hospitals may help improve health care, other measures are equally important. The ACA’s bundled payments and the Hospital Value-Based Purchasing incentive payment program are two examples. You may use the two measures to determine which hospital is the most effective for improving patient safety.